Last Updated on 28 December 2025 by DrElla
Have you noticed that you feel exhausted after meals, crave sugar even when you’re not hungry, or struggle with stubborn belly weight that just won’t budge? You’re not alone — and it’s not “just aging.”
Insulin resistance is one of the most common (and misunderstood) metabolic challenges women face in midlife. It often appears quietly during perimenopause and menopause, affecting energy, weight, mood, sleep, and long-term health.
The good news? With the right knowledge and gentle, consistent changes, insulin resistance can often be improved — and sometimes even reversed.
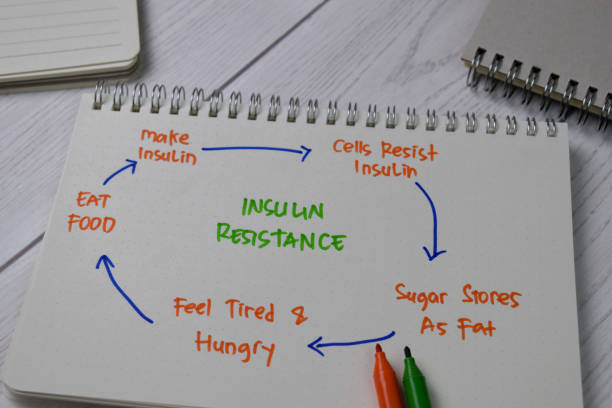
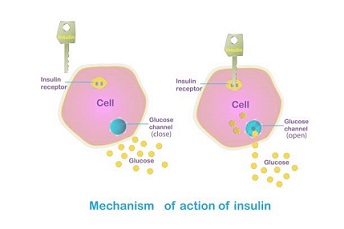
With insulin resistance, those locks become “rusty.”
Your body produces more and more insulin to do the same job — and over time, this leads to:
- Blood sugar swings
- Fatigue
- Inflammation
- Weight gain
- Higher risk of type 2 diabetes
Why Insulin Resistance Is So Common in Midlife Women
During perimenopause and menopause, estrogen levels decline, and estrogen plays an important role in helping the body respond to insulin effectively. As estrogen drops, insulin sensitivity often declines as well.
At the same time, many women experience additional changes that further affect blood sugar balance, including:
-
Increased stress levels
-
Reduced physical activity
-
Slower metabolism
All of these factors can push blood sugar regulation off track.
Chronic stress and unstable blood sugar levels may also contribute to menopause-related sleep problems, especially when sleep is already fragile.
Common Signs of Insulin Resistance You Might Notice
These symptoms are easy to overlook or blame on “getting older,” but they’re important signals from your body:
-
Energy crashes after eating
-
Constant hunger or sugar cravings
-
Difficulty losing weight (especially around the waist)
-
Brain fog or mood swings
-
Irregular periods (if still menstruating)
-
Skin tags or darker patches on the neck or underarms
If several of these sound familiar, it may be time to look deeper.
How to Improve Insulin Resistance Naturally
The foundation is simple — and realistic.
Move Your Body (Gently, but Consistently)
You don’t need intense workouts.
- A 30-minute brisk walk most days can significantly improve insulin sensitivity
- Strength training 2–3 times per week helps muscles use glucose more efficiently
- Even short sessions count
Consistency matters more than intensity.
Eat to Stabilize Blood Sugar
Balanced meals make a powerful difference.
Focus on:
- Protein (eggs, fish, poultry, legumes)
- Fiber-rich vegetables
- Healthy fats (olive oil, avocado, nuts)
Try to reduce:
- Refined carbohydrates
- Sugary drinks
- Highly processed snacks
Eating slowly and mindfully also helps prevent blood sugar spikes.
Prioritize Stress Management and Sleep
Chronic stress raises cortisol, which directly worsens insulin resistance.
Helpful daily habits include:
- Gentle yoga or stretching
- Meditation or deep breathing
- A consistent bedtime routine
Aim for 7–8 hours of quality sleep, as sleep deprivation alone can disrupt blood sugar regulation.
Natural and Holistic Ways to Support Insulin Resistance
Lifestyle changes come first — but many women find additional support through complementary approaches.
Herbal Support
Certain herbs may help improve insulin sensitivity and glucose balance. These are often taken as teas or supplements under professional guidance.
Supplements
Commonly used options include magnesium and chromium. Choose high-quality, third-party-tested products and always consult your healthcare provider.
Acupuncture and Acupressure
These practices may support hormonal regulation, sleep quality, and overall well-being — especially during perimenopause and menopause.
Aromatherapy
While essential oils don’t directly change blood sugar, they support stress reduction — which indirectly helps insulin balance.
Popular choices:
- Lavender (calming)
- Bergamot (stress relief)
- Peppermint or grapefruit (energy support)
Homeopathy
Some women explore individualized homeopathic remedies for sugar cravings, low energy, or hormonal imbalance. A trained homeopath can help identify the most appropriate option.
Mind-Body Practices
Tai Chi or Qi Gong, yoga, meditation and mindful breathing help calm the nervous system, reduce cortisol, and support metabolic balance over time.
Putting It All Together
Think of these steps as layers of support rather than quick fixes.
Start with movement, nourishing food, rest, and stress care, and then explore CAM options to enhance your progress.
When to Talk to Your Doctor
If you suspect insulin resistance, ask about:
- Fasting glucose
- Fasting insulin
- HbA1c
Early testing can help prevent more serious metabolic issues later.
Final Thoughts
Midlife doesn’t have to mean constant fatigue, weight struggles, or feeling “out of balance.”
By understanding insulin resistance — and supporting your body with nourishing food, gentle movement, better sleep, and stress care — you can regain energy, clarity, and confidence.
Your body isn’t failing you.
It’s asking for support.
FAQ – Insulin Resistance in Midlife Women
What causes insulin resistance during menopause?
Hormonal changes, especially declining estrogen, combined with stress, sleep issues, and metabolic slowdown all contribute.
Can insulin resistance be reversed naturally?
In many cases, yes. Consistent lifestyle habits make a significant difference.
Does stress really affect blood sugar?
Absolutely. Chronic stress raises cortisol, which increases blood sugar and insulin resistance.
What is the best diet for insulin resistance after 40?
There’s no single diet — but whole foods, balanced meals, and fewer refined carbs work best for most women.
When should I get tested?
If symptoms persist for months or worsen, testing is a smart next step.
What’s Coming Next
Understanding insulin resistance is the first step — but knowing how to support your body naturally is where real change begins. In the upcoming 5-part guide on natural ways to support insulin resistance, we’ll take a deeper look at gentle, holistic approaches that work alongside your lifestyle. You’ll learn how specific herbs, supplements, stress-regulating practices, mind-body techniques, and supportive therapies like acupuncture or homeopathy can help improve insulin sensitivity and restore balance during midlife. Each part is designed to be practical, evidence-informed, and easy to apply — so you can choose the tools that truly fit your body and your life.