Last Updated on 4 January 2026 by DrElla
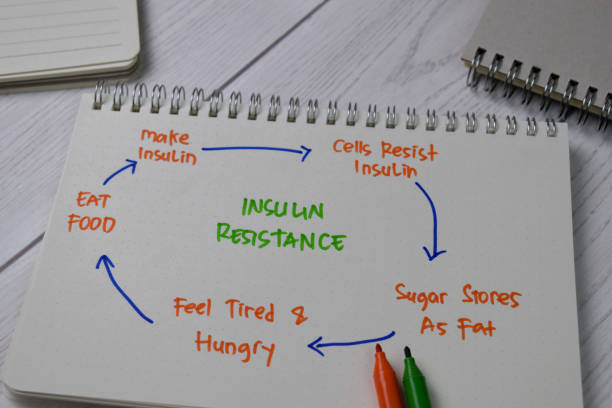
If you’re dealing with insulin resistance and feeling stuck with blood sugar spikes, cravings, or low energy, you’re not alone. Insulin resistance is incredibly common—and the good news is there are natural ways to support your metabolism. Insulin resistance means your cells respond less to insulin. As a result, glucose lingers in the blood, insulin levels climb, and energy feels erratic.
Alongside essentials like nutrition, exercise, and sleep, many people turn to natural remedies for insulin resistance, including herbs and supplements that may help improve insulin sensitivity, balance glucose levels, and ease those stubborn sugar cravings. In this first part of the guide, I break down the most effective, research-backed herbs and nutritional supplements that can support healthier blood sugar and a more stable, energized day.
FRIENDLY REMINDER: This guide is educational. Always check with your clinician, especially if you have a medical condition, or take medication, notably antidiabetic (glucose-lowering) medicines, blood thinners, SSRIs, or antibiotics.
1) Herbal Remedies
HOW HERBS MAY HELP
- Insulin signalling: some herbs act on cell receptors so insulin “key” fits the “lock” better.
- Glucose handling: others slow carb absorption or increase muscle uptake.
- Inflammation & stress: many plants calm pathways that make cells more resistant to insulin.
Cinnamon

- Source plant: Cinnamomum cassia (cassia) and Cinnamomum verum (Ceylon or true cinnamon) are both species of evergreen trees in the family Lauraceae, but they have distinct differences. C. verum is native to Sri Lanka and is known for a more delicate, sweet flavour and aroma, while C. cassia originates from China and is often used as a more robustly flavoured cinnamon.
- What it may do: improve insulin signalling; slow gastric emptying; modest effect on fasting glucose.
- Forms: ground (culinary); extract capsules; tincture.
- Dosing: culinary ½–1 tsp/day; extract 500–1000 mg/day with meals.
- Start/feel: small effects in 2–4 weeks with daily use.
- Cautions: Cinnamomum cassia has higher coumarin → be cautious with liver disease or warfarin (blood thinner). Prefer Ceylon cinnamon (Cinnamomum verum = “true”) if using daily.
Berberine
- Source plant: Berberis aquifolium, the Oregon grape or holly-leaved barberry, is a North American species of flowering plant in the family Berberidaceae. It is an evergreen shrub growing up to 3 metres tall and 1.5 m wide.
- What it may do: activates AMPK2 (“metabolic switch”) = improves glucose use, lipids; may reduce post-meal spikes.
- Forms: standardized capsules (berberine hydrochloride).
- Dosing: 500 mg, 2–3×/day before meals (total 1000–1500 mg).
- Start/feel: Gastrointestinal adjustment common first week; metabolic effects typically 4–8 weeks.
- Cautions: interacts with cytochrome P450 and P-glycoprotein3. Discuss if on glucose-lowering medicines (risk of low glucose), cyclosporine, macrolide antibiotics, or anticoagulants (blood thinners).

Fenugreek

- Source plant: Trigonella foenum-graecum (the scientific name for the fenugreek plant) is an annual herb native to the Mediterranean and Western Asia that is used in both culinary and medicinal applications.
- What it may do: soluble fiber slows carb absorption; may support insulin secretion; helps satiety.
- Forms: seeds (culinary), ground seed, capsules, tea.
- Dosing: 5–10 g/day seeds or 1–2 g extract/day; split doses with meals.
- Start/feel: appetite and post-meal effects within days; glycaemic effects in ~4–6 weeks.
- Cautions: smells like maple syrup; may reduce iron absorption; caution with warfarin (blood thinner) and glucose-lowering medicines.
Gurmar
- Source plant: Gymnema sylvestre, also known as Gurmar or the “sugar destroyer,” is a tropical, perennial climbing vine. The plant is known for its ability to suppress the taste of sweetness and is a popular herb in Ayurvedic medicine.
- What it may do: reduces sugar taste perception; may decrease intestinal glucose absorption; supports pancreatic function.
- Forms: capsules/tea; standardized to ~25% gymnemic acids.
- Dosing: 200–400 mg/day; 30 minutes before sweet foods to curb cravings.
- Start/feel: cravings can shift quickly (days); metabolic effects take weeks.
- Cautions: monitor if on glucose-lowering medicines.

Bitter melon

- Source plant: Momordica charantia (also known as bitter melon or bitter gourd) is a tropical vine producing a bumpy, green fruit that is both a vegetable and a traditional medicinal plant. It is widely used in cooking and valued in folk medicine, particularly for its potential to help manage blood sugar levels and for other reported anti-diabetic, anti-inflammatory, and anti-obesity effects.
- What it may do: “plant insulin”–like actions; may aid glucose uptake.
- Forms: cooked vegetable, juice, capsules.
- Dosing: capsules often 500–1000 mg/day; food uses several times weekly.
- Cautions: can potentiate glucose-lowering meds.
Turmeric/Curcumin
- Source plant: Turmeric is a bright yellow spice that is derived from the underground stems (rhizomes) of the Curcuma longa plant. The plant is part of the ginger family and is grown in warm climates around the world. Turmeric has long been used for its potential health benefits as well as to enhance flavour in culinary dishes.
- What it may do: down-regulates inflammatory pathways that worsen insulin resistance.
- Forms: extract with piperine or phytosome (Meriva/BCM-95 types).
- Dosing: 500–1000 mg curcuminoids/day with fat-containing meals.
- Cautions: gallbladder disease; blood thinners.

Holy Basil (Tulsi)

- Source plant: Holy Basil (Ocimum tenuiflorum), or Tulsi, is a revered medicinal and religious herb native to India that is widely used in Ayurveda. Known as the “Queen of Herbs” and “The Elixir of Life,” it is distinct from the sweet basil used in Western cooking.
- What it may do: adaptogenic stress support; may blunt cortisol-related spikes.
- Forms: tea/tincture/capsules.
- Dosing: tea 1–3 cups/day; capsules 300–600 mg/day.
- Cautions: theoretical additive effects with hypoglycemics.
Practical stacking (choose 1–2 to start)
- Craving control: Gymnema (before sweets) + cinnamon with meals.
- Metabolic push: Berberine (with main meals) + magnesium at night.
- Inflammation + stress: Curcumin (with lunch) + Tulsi tea mid-afternoon.
2) Nutritional Supplements
Magnesium (glycinate/citrate/taurate)
- Why: Magnesium helps your insulin receptors work properly and supports how glucose moves into your cells. Many adults run low on magnesium, especially during times of stress.
- Dose: Most people do well with 200–400 mg at night. Glycinate may support relaxation and sleep, citrate often helps if you struggle with constipation, and taurate can gently support healthy blood pressure.
- Watch: Loose stools often mean the dose is too high. It’s best to take magnesium at least 4 hours away from thyroid medication or antibiotics.
Chromium (picolinate/niacin-bound)
• Why: Chromium helps insulin do its job more efficiently and may even ease carb cravings by supporting stable blood sugar.
• Dose: A typical amount is 200–400 mcg per day with meals.
• Watch: Avoid high doses beyond what’s recommended. If you have kidney concerns, talk with your clinician first.
Alpha-lipoic acid (ALA)
• Why: ALA is a powerful antioxidant that supports insulin sensitivity and helps protect nerves from oxidative stress. Many people find it especially helpful when they feel sluggish after meals.
• Dose: Common doses range from 300–600 mg per day, taken 30 minutes before meals.
• Watch: Because ALA may lower blood sugar, monitor how you feel. Take it 4 hours away from thyroid medication.
Omega-3s (EPA+DHA; fish or algae oil)
• Why: Omega-3s help calm inflammation and support healthy triglyceride levels. They may also improve the way insulin functions throughout the body.
• Dose: Most adults benefit from 1000–2000 mg of combined EPA/DHA4 daily, taken with food for best absorption.
• Watch: If you use blood thinners, check with your doctor. Look for third-party tested oils to avoid contaminants.
Vitamin D3
• Why: Low vitamin D levels often go hand-in-hand with insulin resistance and fatigue. Bringing your levels into a healthy range may support better metabolic balance.
• Dose: It’s helpful to test first, but many adults need 1000–2000 IU daily. Recheck your levels in about 8–12 weeks to see how you’re doing.
• Watch: Too much vitamin D isn’t helpful, so don’t overdo it. Make sure you’re also getting enough vitamin K2 and magnesium, which work together with vitamin D.
Zinc (picolinate/citrate)
• Why: Zinc helps your pancreas store and release insulin. It also supports strong immunity, which is a nice bonus.
• Dose: Many people take 15–30 mg per day with food. For balance, add 1–2 mg of copper for every 15 mg of zinc.
• Watch: Zinc can cause nausea if taken on an empty stomach, so pair it with a meal.
CoQ10 (ubiquinone/ubiquinol)
• Why: CoQ10 fuels your mitochondria—your cells’ energy factories—and helps reduce oxidative stress. This support may improve overall energy and metabolic health.
• Dose: A typical dose is 100–200 mg per day, taken with a meal that contains some healthy fat to boost absorption.
Myo-inositol
• Why: Myo-inositol supports smooth insulin signalling and can improve insulin sensitivity. It’s widely used in metabolic syndrome5 and PCOS6 because it helps regulate glucose levels and encourages hormonal balance.
• Dose: Many adults take 2–4 g per day, usually split into one or two doses with meals for gentler digestion.
• Watch: Most people tolerate it very well. A few may notice mild digestive discomfort. If you already take glucose-lowering medications, check with your doctor first.
Combining Remedies: Using Synergy Wisely
When it comes to supporting insulin resistance naturally, combination remedies can sometimes offer more balanced and noticeable effects than single herbs or supplements alone. Because insulin resistance is influenced by multiple factors—like inflammation, stress hormones, glucose absorption, and cellular energy—pairing complementary remedies can address several pathways at once. For example, cinnamon or fenugreek can help manage post-meal glucose swings, while gymnema may reduce sugar cravings, and curcumin or holy basil can target stress- and inflammation-driven metabolic strain. Nutrients like magnesium, omega-3s, ALA, and berberine can then provide deeper metabolic support by improving insulin signaling and mitochondrial efficiency.
Combination remedies offer a holistic approach by blending several active ingredients that work synergistically to address multiple symptoms at once. These formulations can simplify treatment plans, reduce the number of products needed, and improve user convenience by providing broader therapeutic support in a single application. They are especially useful when several underlying factors contribute to discomfort or dysfunction, allowing for a more comprehensive and streamlined intervention. Many ready-made combination remedies are commercially available, offering pre-balanced formulations that are easy to incorporate into routine care.
As you explore these natural tools for supporting healthier insulin function, remember that this guide is just the beginning. Part 2 of this series is coming soon, where we’ll dive into the next set of complementary approaches — Acupuncture/Acupressure and Aromatherapy. These gentle, holistic therapies can work alongside lifestyle changes and supplements to support metabolic balance in a more complete, whole-body way. Stay tuned!
GLOSSARY
1SSRI = Selective Serotonin Reuptake Inhibitor. It’s a common type of antidepressant that helps increase serotonin levels in the brain to improve mood.
2AMPK =AMP-activated protein kinase. It’s an enzyme that acts like a cellular “energy sensor,” helping your body balance how it uses and stores energy. When AMPK switches on, it supports healthier metabolism, better glucose uptake, and improved insulin sensitivity.
3cytochrome P450 and P-glycoprotein
Cytochrome P450 is a group of enzymes in your liver that helps your body break down medications, supplements, and toxins. Think of it as your body’s chemical “processing system.” Some substances speed it up, others slow it down. When it changes speed, medications may become stronger or weaker than expected.
P-glycoprotein is a transport protein that acts like a tiny “pump” in your cells.
Its job is to push drugs and other substances out of cells, especially in the gut, liver, and brain. If something blocks this pump, medications can build up in your body. If something speeds it up, medicines may clear too quickly.
Together, CYP450 enzymes and P-glycoprotein play a major role in how your body absorbs, uses, and removes medications—which is why some supplements and drugs can interact with each other.
4EPA/DHA: EPA (eicosapentaenoic acid) and DHA (docosahexaenoic acid) are two key omega-3 fatty acids found mainly in fish oil and algae oil. EPA helps lower inflammation and supports heart and metabolic health. DHA supports brain, nerve, and eye function. Your body can’t make much of either on its own, so getting them through food or supplements is often helpful.
5Metabolic syndrome is a group of health problems that often show up at the same time and make it harder for your body to control blood sugar and inflammation. It usually includes high blood sugar, high blood pressure, unhealthy cholesterol or triglycerides, and extra fat around the belly.
Having metabolic syndrome doesn’t mean you’re seriously ill right now. It simply means your body is working harder than it should and your risk for conditions like type 2 diabetes and heart disease is higher. The encouraging part is that simple lifestyle changes—better eating, regular movement, good sleep, and stress management—can improve it and sometimes even turn it around completely.
6PCOS=Polycystic Ovary Syndrome.
It’s a common hormone-related condition that affects people with ovaries, usually starting in the teen or young adult years. PCOS happens when the body makes more androgens (male-type hormones) than usual, which can disrupt normal ovulation: the ovaries may not release an egg every month; small fluid-filled sacs (not harmful) can build up in the ovaries; hormone imbalances affect periods, skin, and metabolism.
Common signs include irregular periods, acne, weight gain or difficulty losing weight, excess hair growth, and sometimes fertility challenges. Many people with PCOS also struggle with insulin resistance, which is why lifestyle changes and certain supplements can help.