Last Updated on 4 January 2026 by DrElla
During menopause, the decline in oestrogen levels leads to measurable changes in the cardiovascular system. These hormonal shifts affect blood vessel function, blood pressure regulation, and lipid metabolism, contributing to an increase in menopause cardiovascular risks.
As a result, women may experience symptoms such as rising blood pressure, heart palpitations, reduced exercise tolerance, fatigue, or shortness of breath. Although these changes are often part of the menopausal transition, they also coincide with a period when the long-term risk of heart disease begins to rise.
Early recognition of cardiovascular symptoms, combined with appropriate monitoring and evidence-based lifestyle or medical interventions, plays a key role in protecting heart health during and after menopause.
GENTLY REMINDER: This article is based on current clinical understanding of menopause-related cardiovascular changes and is intended for educational purposes. Individual risk assessment should always be discussed with a qualified healthcare professional.
Why Menopause Increases Cardiovascular Risks
Oestrogen plays a protective role in the cardiovascular system. It helps keep blood vessels flexible, supports healthy cholesterol balance, and contributes to normal blood pressure regulation.
As menopause approaches and oestrogen levels fluctuate and fall:
-
Blood vessels may become stiffer
-
Blood pressure may gradually rise
-
Cholesterol levels may shift unfavourably
-
The risk of heart disease increases over time
This is why cardiovascular disease becomes the leading cause of death in women after menopause — even though symptoms may be subtle or atypical.
Common Cardiovascular Symptoms During Menopause
Heart Palpitations
Many women describe palpitations as:
-
A fluttering or pounding heartbeat
-
A racing heart without physical exertion
-
The sensation of skipped or irregular beats
Hormonal fluctuations can affect the autonomic nervous system, making the heart more sensitive to stress hormones like adrenaline. Although palpitations are often harmless, they can feel frightening.
When to check:
If palpitations are frequent, prolonged, or accompanied by dizziness, chest pain, or breathlessness, medical evaluation is important.
Chest Pain or Chest Discomfort
Chest discomfort during menopause may feel like pressure, tightness, or aching. It can sometimes resemble anxiety or panic-related sensations.
However, falling oestrogen levels can also lead to:
-
Reduced vessel flexibility
-
Early atherosclerosis
-
Microvascular dysfunction (small-vessel heart disease)
Important! In women, heart-related chest symptoms may appear as fatigue, nausea, jaw or upper-back discomfort rather than classic chest pain.
Shortness of Breath
Breathlessness during menopause may be linked to:
-
Reduced cardiovascular fitness
-
Elevated blood pressure
-
Anxiety or panic episodes
However, persistent or activity-related shortness of breath should always be assessed to rule out heart or lung conditions.
Dizziness or Light-Headedness
Feeling faint or off-balance can occur due to:
-
Blood pressure fluctuations
-
Dehydration
-
Heart rhythm irregularities
If dizziness occurs together with palpitations or near-fainting episodes, further evaluation is recommended.
Fatigue and Reduced Exercise Tolerance
New or worsening fatigue — especially during activity — is common in menopause.
However, women often experience fatigue as an early symptom of heart disease, rather than chest pain.
Poor sleep plays a major role here. Thus, poor sleep and frequent night waking can intensify palpitations and fatigue, making night waking in menopause a concern that shouldn’t be ignored.
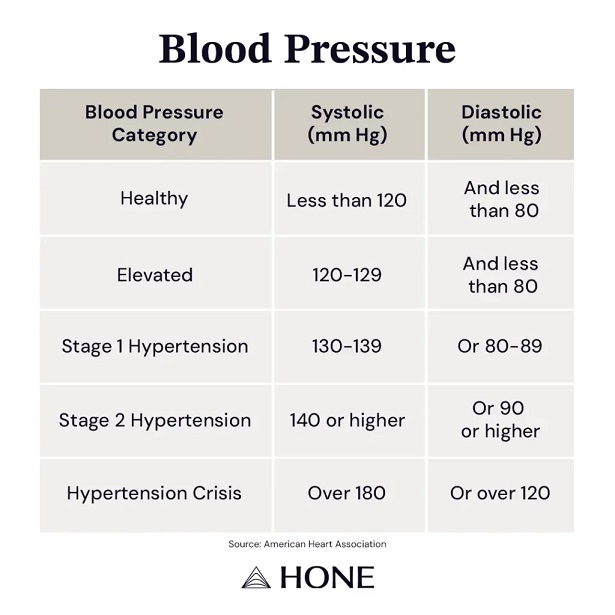
High Blood Pressure in Menopause
High blood pressure often develops without noticeable symptoms.
As oestrogen declines:
-
Blood vessels become less elastic
-
Vascular resistance increases
-
Blood pressure rises more easily
Regular monitoring is essential, even if blood pressure was normal earlier in life.
Swelling in the Legs or Ankles
Mild swelling may be related to inactivity or hormonal changes.
Persistent swelling, however, may indicate impaired circulation or heart strain and should be evaluated.
Hot Flashes Triggering Heart-Like Symptoms
Hot flashes can cause:
-
Rapid heartbeat
-
Sweating
-
Chest tightness
These episodes may mimic panic attacks or heart symptoms but are driven by changes in the brain’s temperature and cardiovascular regulation.
Why Cardiovascular Risk Increases After Menopause
Loss of Oestrogen Protection
Oestrogen helps:
-
Maintain healthy blood vessels
-
Reduce plaque formation
-
Regulate cholesterol
Its decline increases the risk of coronary heart disease, heart attack, and stroke.
Unfavourable Cholesterol Changes
-
LDL (“bad” cholesterol) increases
-
HDL (“good” cholesterol) may decrease
-
Triglycerides may rise
Weight Gain and Fat Redistribution
Abdominal (“belly”) fat increases metabolic and cardiovascular risk.
Insulin Resistance and Metabolic Syndrome
Oestrogen decline affects glucose metabolism, increasing the risk of type 2 diabetes and metabolic syndrome.
SOME RECENT SCIENTIFIC FACTS
Over the last two decades, we’ve learned a lot about
How menopause contributes to heart health
- For example, menopause-related hot flashes and night sweats have been linked to a greater risk for high blood pressure and other cardiovascular risk factors.
- Research also shows depression during the menopause transition is strongly linked to higher cardiovascular disease risk.
- Also, studies show that women who go through menopause early (before age 45) tend to have more heart health issues later in life compared to those who reach menopause around age 50. However, experts still debate how significant this effect is and exactly how early menopause impacts heart health.
When to See a Doctor
Menopause-Related versus Heart Disease Symptoms
| Symptom | Menopause-Related | Possible Heart Disease |
| Palpitations | Sudden, brief episodes; often triggered by stress, caffeine, or hot flashes. Usually resolve quickly. |
Persistent or irregular palpitations, especially with dizziness or chest pain. Could indicate irregular heart rhythm (e.g., atrial fibrillation). |
| Chest Discomfort | Often mild, brief, linked to anxiety or hot flashes. Not exertion-related. | Pressure, heaviness, or tightness; triggered by physical activity or emotional stress. May radiate to jaw, arm, back. |
| Shortness of Breath | Can occur during hot flashes or anxiety. Mild and resolves at rest. | With exertion or at rest. Progressive. Could signal heart failure or coronary artery disease. |
| Fatigue | Common in menopause due to poor sleep, mood changes, or hormonal shifts. Improves with rest. | New or worsening fatigue, especially with activity. May indicate heart muscle dysfunction or poor circulation. |
| Dizziness or Light-headedness | May occur during hot flashes or when standing up quickly (blood pressure drop). | Persistent or with palpitations — could suggest irregular heart rhythm (arrhythmia), low cardiac output, or heart valve problems. |
| Sweating | Sudden and intense (hot flashes), not linked to exertion. | Cold sweats with chest discomfort — more concerning for heart attack. |
| Swelling | Mild, cyclic, or related to inactivity. | Persistent swelling in legs or ankles — may suggest heart failure or poor circulation. |
Red Flags That Need Medical Evaluation
Seek medical advice if you experience:
- Ongoing chest pain or pressure
- Breathlessness with minimal effort
- Persistent palpitations
- Fainting or near-fainting
- Unexplained fatigue
- Rising blood pressure
How Doctors Evaluate Cardiovascular Symptoms
Doctors may use:
-
ECG (heart rhythm assessment)
-
Echocardiogram (heart structure and function)
-
Stress testing
-
Holter monitoring
-
Blood tests (cholesterol, thyroid, anaemia markers)
FAQ – Cardiovascular Risks in Menopause
Are heart palpitations normal during menopause?
Yes, they are common and often linked to hormonal fluctuations, but persistent or severe palpitations should be evaluated.
Can menopause cause high blood pressure?
Yes. Declining oestrogen affects blood vessel flexibility, increasing the likelihood of hypertension.
Is fatigue during menopause always hormonal?
No. While hormones play a role, fatigue can also signal cardiovascular issues, especially if it worsens with activity.
Can lifestyle changes really help heart health in menopause?
Absolutely. Diet, movement, stress management, and sleep quality significantly reduce cardiovascular risk.
Key Takeaway
Cardiovascular risks in menopause increase due to hormonal and metabolic changes.
Symptoms such as palpitations, rising blood pressure, fatigue, or breathlessness deserve attention — not fear.
With awareness, regular monitoring, and supportive lifestyle habits, women can protect their heart health through menopause and beyond.


